
 Ever since he was young, Ben White knew he wanted to fly helicopters for the Navy. Ben grew up watching his father ride helicopters as a flight paramedic, and seeing his uncle fly helicopters for the Navy. The only thing stopping him was the idea of being in flight school for so long.
Ever since he was young, Ben White knew he wanted to fly helicopters for the Navy. Ben grew up watching his father ride helicopters as a flight paramedic, and seeing his uncle fly helicopters for the Navy. The only thing stopping him was the idea of being in flight school for so long.
“After graduating college, I had a job that I was absolutely miserable at, kind of a dead-end desk job, and I had always been afraid of the time commitment to flying; eight years after you get your wings. Getting your wings takes anywhere from two to three years, so it’s 10 years total. So at 20, I wasn’t super excited about signing away 10 years of my life. But after about four months of this desk job, 10 years didn’t seem quite as scary anymore. So I called up a recruiter and it was definitely the best decision I ever made.”
At the age of 25, he was soaring higher than ever with that decision, but after Ben turned 26 in late March 2015, his diagnosis in May grounded his flight dreams.
“Starting in late March, I was having a lot of abdominal pain and discomfort. I had one particular weekend, I remember, where I pretty much couldn’t get out of bed, all day Sunday. I went to my doctor the next morning. In the Navy, I had a flight doctor who’s assigned to my squadron. A big part of their job is to, of course, keep you safe, but also to protect your career because the medical standards for aviation are very high. Their approach is they start things slow, they’re not going to immediately jump to the deepest, darkest conclusion. That being said, my flight doctor was still my number one cheerleader, getting me real help when I needed it.”
Since there was no access to a CT machine, Ben’s flight doctor did a work-up and an X-ray. He was sent home with the diagnosis  of constipation and given some laxatives. Things seemed fine when he got home and he was starting to feel better by Monday. “It felt like an isolated incident, and he kind of said, ‘If anything gets worse, keep an eye on it, get back to me.’”
of constipation and given some laxatives. Things seemed fine when he got home and he was starting to feel better by Monday. “It felt like an isolated incident, and he kind of said, ‘If anything gets worse, keep an eye on it, get back to me.’”
Out of nowhere, Ben had a couple days where his fever spiked and he noticed that he was having a lot more bowel movements a day. His energy started to deplete as well, but simply chalked it up to his busy schedule and being so young. “I had a lot less energy, but at the same time, I was in a new squadron, flying my new helicopter, and I was working out a lot. So it was kind of those, ‘Yeah I’m tired all the time, but I’ve got a lot in my schedule. I’m very stressed.’”
Ben’s sister, who is a nurse practitioner, was visiting him over Easter weekend and noticed his drastic weight loss. He had kept her updated on his health from the beginning and she knew it was worse. “She came and visited me in Florida and I guess I hadn’t really noticed but I had lost quite a bit of weight. She said, ‘You really need to go see someone. There’s something deeper that’s wrong here.’”
Little did Ben know, this was just one bump in the rollercoaster that would be his diagnosis. He went back to his doctor, who was actually out for a few weeks, and instead met a different doctor on duty. The doctor had simply told him to cut some certain foods out of his diet and check back in two weeks to see what would happen. After a week of seeing the doctor, Ben knew something was wrong when he wasn’t sleeping through the night and constantly waking up in the middle of the night to use the bathroom. “This was when I said, ‘This isn’t working, I need to see what else is going on.’”
 Ben went back to his doctor and they were able to do a complete work-up, including a CT scan and stool samples, to try and rule out anything. “At this point, they were thinking potentially Crohn’s or something like that, which also would’ve been career ending for me, but at this point, getting healthy was still priority.” Ben had to travel across town to another Navy base to get the CT scan and work-up. “And it was at 7 a.m. the next morning, basically as soon as the doctor got in, he called me, ‘Hey, you need to head to the ER on the Navy base, and be ready for emergency surgery.’ His direct quote was that ‘it looked like a grenade had gone off in my colon.’”
Ben went back to his doctor and they were able to do a complete work-up, including a CT scan and stool samples, to try and rule out anything. “At this point, they were thinking potentially Crohn’s or something like that, which also would’ve been career ending for me, but at this point, getting healthy was still priority.” Ben had to travel across town to another Navy base to get the CT scan and work-up. “And it was at 7 a.m. the next morning, basically as soon as the doctor got in, he called me, ‘Hey, you need to head to the ER on the Navy base, and be ready for emergency surgery.’ His direct quote was that ‘it looked like a grenade had gone off in my colon.’”
While sitting in the ER waiting room, the surgeon and ER doctor had came out and saw that Ben wasn’t who they were expecting. “They were like, ‘Oh, you’re the guy! You look way too healthy. We expected you to be on your last rattling breath, based on your CT.’ So basically they decided not to offer it. They sent me home with antibiotics. They quoted diverticulitis, saying I simply had an enflamed colon. And it was so enflamed that we knew we couldn’t get a scope in, for risk of perforation. So the plan was to put me on antibiotics and see if it goes down and then we’d get a scope.”
But Ben was back the next day, having not slept at all. The doctor who saw him simply said that he needed to a few more days because the antibiotics hadn’t kicked in yet. Ben made them admit him and observed him all weekend. “But the whole time, I had these doctors who were just so highly skeptical. I don’t know what they thought, but they didn’t think I was as ill as I actually was.”
Ben was discharged on Sunday after no change and no bowel movements. He was home for two days before heading back to the ER with severe pain. “It was beyond. It had gone from mild abdominal discomfort to extreme pain. I was nauseous; I wasn’t really eating. I hadn’t had bowel movement in about 4-5 days.”
They sent him home again, this time with laxatives, which Ben said almost killed him. “At this point, it turns out my tumor had entirely blocked my colon – it was completely obstructed. So I went home, one more night, took some laxatives and spent the entire night in misery. The next morning, I had my roommate drive me back and suddenly had a surgeon who took me seriously and admitted me right away.”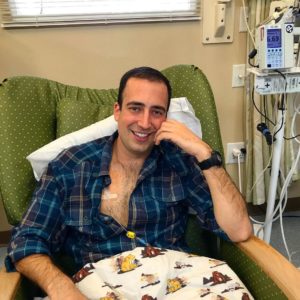
There were more CTs, but because his colon was so enflamed, they couldn’t see a clear tumor or what was wrong. Everyone was simply waiting, hoping eventually to get a clear scan of his colon. They even tried giving him enemas, but when that didn’t work, they theorized that his colon was so diseased that it had simply closed on itself. With his sister being a nurse practitioner, and his parents both being nurses, Ben came out and asked, “Okay, how are we writing off colon cancer?” His earlier encounters with different doctors all told him he was too young to have colon cancer.
“At this point, I had lost 30 pounds without even trying. I had every red flag in the book. And I told them this every time I went in.” His surgeon agreed, but didn’t want to jump to conclusions until he was sure. They decided to do an exploratory laparoscopic surgery to get a clear sense of what was actually happening. Ben’s doctor found a lemon-sized tumor in his sigmoid colon and removed about 6.5 inches of his colon. “So basically I went from going in for an exploratory surgery to waking up to a colostomy and cancer diagnosis, which was a little bit jarring. So from there, I spent another week in the hospital recovering from the surgery.”
Ben was on his way to be discharged when he contracted Clostridium difficile, or C. Diff, and had to be in the hospital for another week before being able to meet his oncologist and start chemotherapy.
Given his age and diagnosis of stage IIIb colon cancer, it was suggested he do the full 12 rounds of FOLFOX. Even though he came out surgery with a clean scan, he chose to be more cautious of his health. Because Ben was stationed in Florida and his entire family was in California, the Navy decided to send him home to continue his treatment. It worked out well because although he had friends willing to sacrifice time for him, they couldn’t constantly take time off from their jobs to help him get to his chemo appointments. Between rounds 2 and 3, Ben packed up his car and his dog, Izzy, and drove from Florida all the way to Northern California to move back in with his parents and make it in time for his next round of treatment. “I was very lucky, both my parents were just recently retired, my sister had a month and a half off where she was going to travel in between two different jobs. She had found a new job at Stanford and quit her old one at the hospital. Instead of traveling, she came and helped take care of me so my family was able to take turns.” He made it in time for his next round, but knew it was difficult, especially coming off of treatment.
 Ben finished his last round in early December 2017, had a clear scan, and was declared NED. In late January 2018, he went in to get a reversal of his ostomy, and ended up staying longer than expected. “I had C. Diff the first time I was in the hospital, it took me an extra week. This time I had pancreatitis, so my 2-3 days in the hospital for the ostomy reversal turned into 8-9 days. But by March, I had recovered and back to a normal state of being able to exercise lightly and things like that.”
Ben finished his last round in early December 2017, had a clear scan, and was declared NED. In late January 2018, he went in to get a reversal of his ostomy, and ended up staying longer than expected. “I had C. Diff the first time I was in the hospital, it took me an extra week. This time I had pancreatitis, so my 2-3 days in the hospital for the ostomy reversal turned into 8-9 days. But by March, I had recovered and back to a normal state of being able to exercise lightly and things like that.”
Around this time, the Navy had officially started their medical review process for Ben. It was a long process, having to determine whether or not Ben was fit for duty and if he wasn’t, what type of pensions and benefits he would get. Ben got the decision on a Sunday, and as of Monday, October 29, he was officially separated from the Navy.
Ben credits his flight doctor, who believed his every word that he was sick, and his family background and knowledge with his decision to take his diagnosis in his own hands. With his parents and sisters as nurses, and his uncle as a doctor, he knew that if they were constantly asking for updates on his health, he had to be proactive. With his father specifically being a GI nurse, Ben said growing up with poop conversations at the dinner table was very common. With no family history of colon cancer, Ben was tested in Florida and in California for any sort of genetic mutation markers as well as Lynch syndrome, but it all came back negative.
Ben’s total time with the Navy, even through treatment, was two weeks short of four years. When he was diagnosed it was about two and a half years. He spent two years in flight school, got his wings of gold in December of 2016, and became an official Naval Aviator after extensive training. Jacksonville was his permanent duty station where he learned to fly his MH-60.
Ben is currently spending his time traveling around Europe, even taking a trip to a small Jewish village in Eastern Germany to explore the roots of his maternal great-grandparents’ history during World War II and partake in a ceremony the village holds for descendants of the Jewish families that lived there. Ben is also keeping himself busy and bringing positivity into his life, by helping his high school friends, Matt and Nate, who are the co-founders of PEAR Cards, which he says is a passion project of theirs.
PEAR stands for “Positive Engagement And Response.” PEAR Cards were started with Nate and his mother when he was young. Growing up in a single parent home, Nate’s mother tried her best to communicate and talk to her son after school. After realizing that his answers weren’t enough, she started writing prompts down onto slips of papers and put into a “Positivity Pot.” Positively-focused questions and prompts, such as, “The best thing that happened to me today was___.”
After seeing the prompts getting used by people of all ages at a friend’s college graduation party, Nate and Matt knew this was something they had to share with everyone. Ben joined to help create and design the concept and physical appearance of PEAR Cards. After raising $19,000 on Kickstarter, they were able to ship some out to their biggest supporters, and sell the surplus they had to schools, therapists, and even a foster agency in Fresno, California, with nothing but positive feedback on how much the cards are making an impact on positivity and mental health.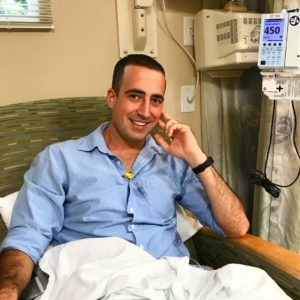
Besides his passion project, Ben will be featured in The Colon Club’s 2019 On the Rise Magazine, and will be involved in Fight Colorectal Cancer’s 2019 Call on Congress in March to bring more awareness to colon cancer in young adults.
“In terms of plans: just keep sharing my story. I’m very much an open book with anyone I meet about it, because if my story enables one person to get diagnosed sooner than I did, then I’ll count that as a win.”
RETURN TO FACES OF BLUE Learn More About Young Adult Colorectal Cancer
